Member Engagement
SDOH: Overcoming Obstacles to Better Health Outcomes
SHARE

As benefits professionals strive to help employees and their families stay healthy, while also controlling claims costs, social determinants of health (SDOH) stand as a significant and stubborn barrier.
The World Health Organization defines SDOH as “the conditions in which people are born, grow, work, live, and age, and the wider set of forces and systems shaping the conditions of daily life.” The Kaiser Family Foundation (KFF) groups these nonclinical health factors into six broad categories:
All these factors can have a negative impact on health. Researchers at the University of Wisconsin’s Population Health Institute created a model for measuring and ranking U.S. counties on health outcomes and contributing factors. Their model attributes as much as 50% of outcomes to a combination of clinical care and lifestyle behaviors. The remaining 50% are attributable to SDOH, including a person’s physical environment, plus a range of social and economic factors, from income and education level to family and community support.
With SDOH playing such a major role in health outcomes, HR teams and benefits advisors face the persistent challenge of how to solve for them in member populations. Navigation Insider recently explored the subject of SDOH with Quantum Health’s clinical team. The takeaways can be useful as you explore ways to tackle these powerful, but often elusive, factors affecting your members’ health.
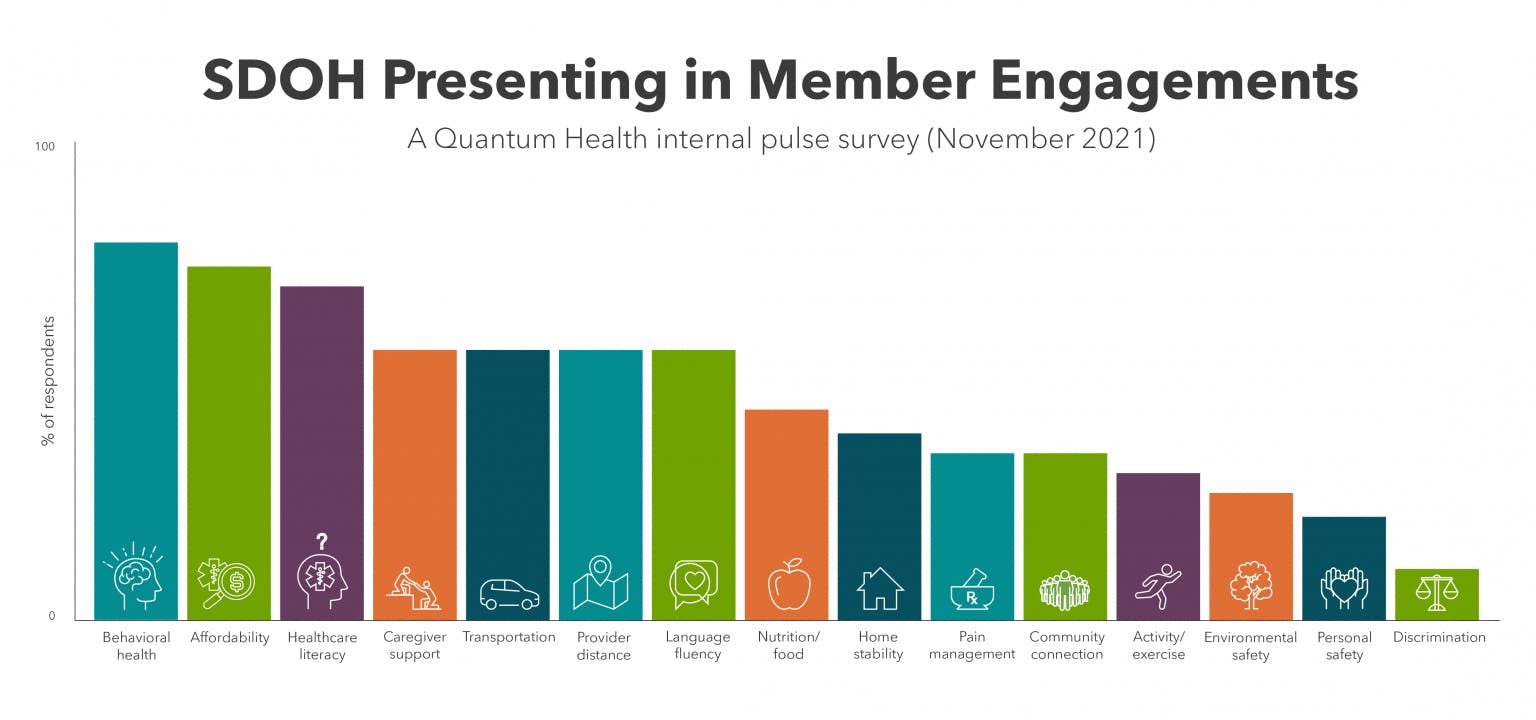
We surveyed our clinical team leaders to gauge which specific SDOH might be present in Quantum Health’s thousands of daily engagements among more than 2 million members.
Our survey broke KFF’s categories into 15 more-specific SDOH challenges. The findings reveal that today’s members face the gamut of SDOH issues. All 15 challenges have surfaced in member engagements during the past 12 months. The four we encounter most often are:
Dr. Michael C. Sokol, Quantum Health’s senior vice president, clinical strategy, said he empathizes with HR leaders and benefits advisors, because SDOH pose multiple obstacles to traditional benefits solutions. Since SDOH are so varied, there’s no all-purpose point solution. SDOH also aren’t limited to a demographic or socioeconomic cohort — literally anyone can find themselves facing a barrier to physical or emotional health. When they do, it’s often not something they’re eager to share with HR colleagues, or even with a primary care provider.
To make progress on addressing SDOH, Sokol said, employers can consider taking steps to expand benefits coverage, especially in areas of your plan where a focused enhancement could make a difference. Using our pulse survey as an example, that might mean increasing the number of mental health counseling sessions covered by an EAP. Or it can involve working with network and telehealth partners to ensure members facing access barriers have virtual care options. Employers would want to conduct original research to learn which SDOH are most common or urgent among their own members.
Beyond considering plan changes, Sokol said, a self-insured employer’s member services model and engagement strategy play a pivotal role in spotting and solving members’ specific SDOH issues.
Using Quantum Health’s core healthcare navigation and care coordination services as an example, he said, members with SDOH challenges receive wide-ranging support from our Care Coordinators, including our Personal Care Guide nurses. The nurses’ clinical expertise and empathetic benefits guidance combine to build trusting relationships, making some members more comfortable disclosing barriers to their well-being. Often that means our nurses can start problem-solving an SDOH issue during the same chat session or call when it first surfaces. Examples include:
Sokol said Quantum Health’s engagements with members offer frequent reminders of just how nuanced SDOH challenges — and the highly personalized solutions — often become. Here are a few examples:
“These stories always remind me that, for many SDOH scenarios, there just isn’t a conventional, off-the-shelf answer,” Sokol said. “It requires being absolutely committed and creative in coming up with ways to help that member in need. Not all member services models are built, or have the resources, to come up with those types of solutions. And they can ultimately have a huge impact on members’ health and quality of life.”
Given the variety and complexity of SDOH, and the highly individualized scenarios that play out in members’ lives, Sokol said SDOH will continue to pose challenges for employers and their benefits plan. But, he added, there are ways to make consistent, meaningful impact and progress.
Those options include adopting an enhanced member services and engagement model, which helps identify and problem-solve for SDOH on an ongoing, member-by-member basis. SDOH insights gained from those engagements create a powerful data set that employers can use to inform future benefits plan enhancements. Combined, these approaches should yield better health outcomes, despite the complexities posed by SDOH.